Over the past few years, measles has become ubiquitous with another word: panic. In America, there have been more than 1,000 reported cases of measles in 28 different states this year, with enormous effects on many communities throughout the country.
But why is this all happening now? Why has measles made such an abrupt and noticeable return after having been declared eliminated from the United States in 2000? The Centers for Disease Control (CDC) says the number of measles cases is at the highest level in 27 years.
What Is Measles?
To start, let’s first understand the subject at the center of this discussion, the measles virus. Measles, or rubeola, is a highly contagious viral infection that starts in the respiratory system. The virus spreads through the air, normally through a cough or a sneeze.
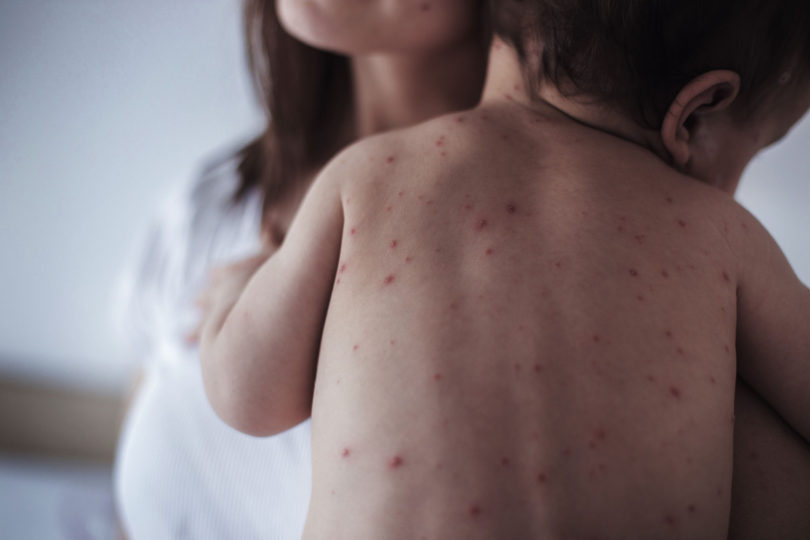
Because of this relatively simple pathology, an unvaccinated person has a 90 percent chance of contracting measles if he or she is near an infected person. It generally takes 10 to 14 days for the appearance of symptoms, which can include cough, runny nose, inflamed eyes, sore throat, fever and a red, blotchy skin rash. Complications are usually much more severe in infants and young children, as well as in people who are immunocompromised.
“It’s one of the most contagious infectious diseases,” says Dr. Nipunie Rajapakse, a Mayo Clinic pediatric infectious diseases specialist, on the Mayo Clinic’s website. “Measles infection is spread through the airborne route, which means you have to inhale the infectious virus. And because it is very tiny droplet nuclei, those can remain suspended in the air for up to two hours after someone with measles has left an area.”
Left untreated, measles can cause severe health complications, such as pneumonia and encephalitis, which is swelling in the brain and can lead to permanent brain damage. The CDC estimates that 1 in every 20 children who contract measles will also get pneumonia, which is the most common cause of death in young children with measles.
Before a vaccine was developed and made available to the public in 1963, nearly everyone got the measles. In 1971, a combination vaccine — the MMR — was released to protect against measles, mumps and rubella. Today, it’s the vaccine most often associated with measles.
Spreading Across The Country
Currently the measles outbreak is mostly concentrated in parts of New York, New Jersey, Michigan and Washington. Areas such as New York’s Rockland County and New York City, where there was an outbreak in Brooklyn’s Orthodox Jewish community, have even declared states of emergency. However, there are measles cases all throughout the U.S., posing the threat of an even greater outbreak should the virus continue to spread.
So what is causing this outbreak of measles in the United States? The most likely culprit would be an unvaccinated individual who traveled out of the country and contracted the measles virus. Because measles has an incubation period of 9 to 12 days, it’s feasible that one wouldn’t know he or she had contracted the disease until back in the States. Once back home, any unvaccinated individual that the contagious person came in contact with could catch the disease, further spreading it.
Last year, according to the CDC, outbreaks in New York and New Jersey were associated with travelers who brought measles from Israel, where there is a large outbreak. Europe, meanwhile, is in the middle of its own measles epidemic, with over 34,000 reported cases in 42 different countries in just the first two months of 2019, according to the World Health Organization (WHO).
It’s been shown that measles can be a plane ride away. Last month, a child contracted measles while out of the country and returned through Dulles International Airport, prompting a health advisory in Northern Virginia to locate people who might have been exposed. It wasn’t clear at the time whether the child had been vaccinated.
The Need For Herd Immunity
The rise of anti-vaccination movements and the plethora of states that have personal exemption laws regarding vaccines have contributed to America’s inability to achieve herd immunity against measles. Herd immunity is the principle that 100 percent of a population does not need to be immunized if the vast majority of a population is vaccinated and immune to a particular disease. Then, there’s no way for the disease to travel if introduced into the community.
“When measles is imported into a community with a highly vaccinated population, outbreaks either don’t happen or are small,” Nancy Messonnier, the director of CDC’s National Center for Immunization and Respiratory Diseases, said in a news briefing earlier this year. When measles shows up in a community with low vaccine coverage, “it is difficult to control the spread of disease.”
The less infectious a disease, the lower the vaccine coverage needed for herd immunity. Herd immunity is of great importance to public health since there are certain subsets of the population who cannot be immunized for either medical or religious reasons. For a tremendously infectious disease such as measles, a vaccination rate of around 92-95 percent is the minimum required for herd immunity, according to the CDC.
As of 2016, according to the CDC, the U.S. was at 91.1 percent of young children immunized. While this number seems high, it does not reach the minimum recommended percentage of immunized children to achieve herd immunity, something that is very likely contributing to the outbreak that the U.S. is currently experiencing.
For children who can’t be vaccinated, getting the measles “can be fatal or wind up causing serious complications,” says Dr. Yvonne Maldonado, a pediatric infectious disease expert at Stanford University School of Medicine, in Science News. “That’s a real fear for [these] families.”
How Should People Protect Themselves Against Measles?
Even if someone has received a measles vaccine, one dose is only 93 percent effective at preventing the disease, says the CDC. A booster can be administered to increase the effectiveness even more. Boosters work in the same way that vaccines work, re-exposing people to the disease so that they are able to create more antibodies to fight the disease should they come into contact with it. The American Academy of Pediatrics (APP) recommends that children receive two doses of the MMR vaccine between ages 1 and 6.
However, the effects of vaccines can lose their potency in the body over time. Antibodies that were created when the vaccine was first administered can die off over the years so their levels are lower. By receiving a booster, individuals can increase their chances of staying healthy in a measles outbreak by ensuring that their body is well equipped to fight measles.
“A third dose of [MMR] vaccine isn’t going to harm you,” says Dr. Joseph Baust Jr., a pediatrician at TPMG James River Pediatrics in Newport News, Va.
Probably the largest factor we’re fighting is misinformation. According to the Red Book, a leading text on pediatric infectious diseases, the MMR vaccine is very safe and is 99 percent effective at preventing measles when given in two doses.”
The best course of action is to not travel to areas where there are recent documented cases of measles, especially if travelling with an unvaccinated individual. Places like Western or Southern Europe where the outbreak is not as prominent, or states such as Maine, South Carolina or Hawaii where no measles cases have been reported are safer choices than others.
Additionally, experts say, unless a medical condition prevents it, receiving the proper, recommended vaccinations is an important step to ensure that the measles outbreak, and any other potential preventable, infectious disease outbreak, spreads as little as possible.
“We cannot say this enough,” U.S. Health and Human Services Secretary Alex Azar said in a statement in June when the number of cases hit 1,000. “Vaccines are a safe and highly effective public health tool that can prevent this disease and end the current outbreak.”