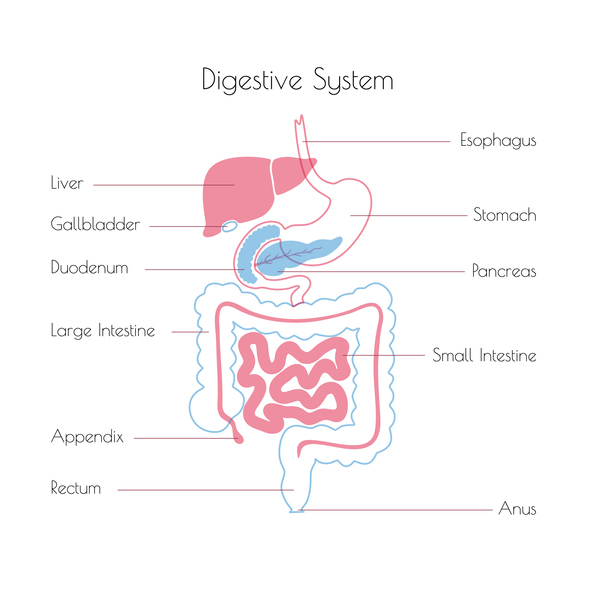
August marks Gastroparesis Awareness Month, which is a good time to shed light on a stomach or gastric disorder that can cause very serious and even life-threatening health problems.
Gastroparesis (gas-tro-puh-REE-sis), or delayed gastric emptying, is a disorder in which stomach muscles fail to contract in a coordinated manner, and in turn fail to propel the ground-up food into the small intestine. While mild slowing of motility can bring health benefits by increasing satiety and aiding in weight management, food delayed too long in the stomach can make us literally sick to our stomachs.
Awareness of delayed gastric emptying generally occurs during or after a meal, resulting in symptoms such as nausea and vomiting, or feeling unusually full very quickly. Other gastrointestinal distress can include bloating, heartburn and stomach pain. If left untreated, gastroparesis can lead to severe dehydration and malnutrition as well as obstruction caused by hardened food that has overstayed its welcome. Anyone experiencing symptoms that are ongoing and cause excessive weight loss should see a doctor.
The most common cause of gastroparesis is damage to the vagus nerve, which controls the stomach muscles. Diabetes is the most common cause of gastroparesis as it damages the vagus nerve, preventing normal signals to the stomach muscles. Abdominal or esophageal surgery also can cause vagal nerve injury. Medications such as antidepressants and narcotics can inhibit normal gastric motility, as can nervous system disorders such as Parkinson’s disease and multiple sclerosis. Less common causes of gastroparesis include Scleroderma (an immune system disorder that attacks and hardens the connective tissue surrounding the internal organs, damaging the stomach muscles) and hypothyroidism.
If gastroparesis is suspected, a gastroenterologist can perform tests to confirm the diagnosis. These include endoscopy, to examine the stomach lining for abnormalities and any obstruction, and special tests that measure gastric emptying of a standardized meal.
Solutions for Smoother Food Movement
No cure exists for gastroparesis, but there are treatments that help. Dietary modifications are the best first step, including avoiding high-fat foods; eating smaller, more frequent meals; or adopting a liquid diet. A few medications can also help improve gastric motility and, rarely, surgical intervention—making a short cut from the stomach to the small intestines—can help food move more smoothly.
Malnutrition can be debilitating with gastroparesis, and adding probiotics, which pass through the stomach intact, can improve absorption of vitamins, nutrients and protein.
Although procedures and medications can stimulate stomach muscle contraction, natural approaches such as dietary changes and nutritional supplementation can avoid the unpleasant side effects and risks possible with invasive practices and taking synthetic drugs.
Probiotic supplements have proven to be effective in addressing small intestinal bacterial overgrowth (SIBO), the presence of excessive bacteria in the small intestine that often accompanies gastroparesis. Because disturbances in gut immune function increase the likelihood of developing SIBO, introducing live strains of beneficial bacteria such as Lactobacillus can help balance gut flora and reduce inflammation that causes gastrointestinal distress. When antibiotics are prescribed to treat the overgrowth of harmful bacteria, probiotic supplementation can also ease side effects such as antibiotic-associated diarrhea (AAD) that can only exacerbate the symptoms associated with gastroparesis.
Because diabetes is the most common factor associated with developing gastroparesis, it makes sense to look at ways to prevent or improve the condition. Obesity, which is linked to diabetes and other metabolic problems, can be prevented with regular exercise and avoiding highly processed foods that hinder the digestive system and the body’s ability to heal itself. All-natural probiotic supplementation can help keep the intestinal microbiome balanced and free from chronic inflammation, which lies at the root of many ailments and diseases, from allergies and autoimmune disorders to cancer.