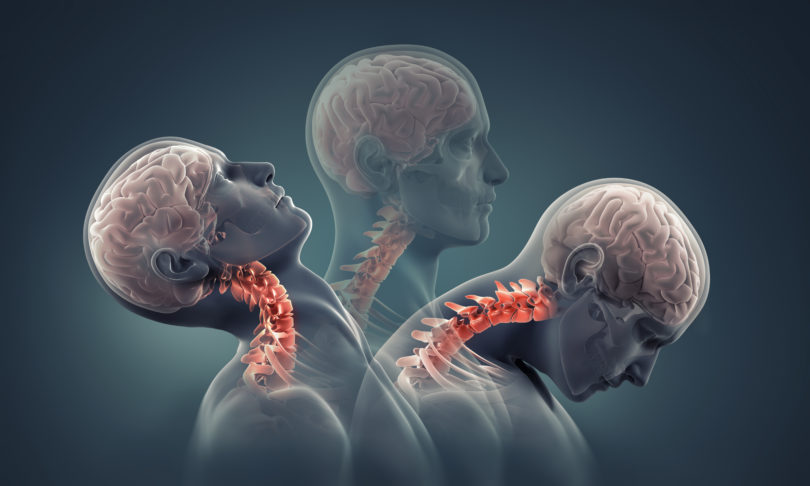
The stereotypes about whiplash are simple: high-speed car crash followed by neck pain, quick diagnosis and medicine-plus-neck brace for healing.
In fact, the common injury often is anything but straightforward. Whiplash can occur with minor impact, symptoms can appear away from the neck, internal damage can be difficult to pinpoint on imaging tests and treatment may need to be multi-faceted, with a neck brace one of the least effective options.
“Some people have suffered for months by the time they get to me,” says Dr. Scott Bradley, a physical medicine and rehabilitation physician with Hampton Roads Orthopaedic & Sports Medicine in Williamsburg. “They may have been to three or four different doctors and either had medicine thrown at them or been told there’s nothing physically wrong with them. You can see the frustration.”
Whiplash is caused by a sudden acceleration and deceleration of the head, which damages ligaments, cartilage or muscles in the neck. An injury can occur at speeds as low as 5 miles per hour; more than 80 percent of people in car accidents suffer some degree of whiplash, Bradley says.
While neck pain and stiffness are common signs, other lesser-known symptoms can appear in the days and weeks after impact. Those include headache, dizziness, fatigue, insomnia, blurred vision, tinnitus, memory and concentration problems, and pain or numbness in the shoulders, arms, jaw and upper back. Issues may be linked to neck damage and/or a whiplash-induced concussion.
Without prompt treatment, people may run the risk of developing chronic pain conditions, says Dr. Robert Pinto, a chiropractor at Pinto Chiropractic & Rehabilitation in Williamsburg.
“It is very important to control pain and inflammation as soon as possible,” Pinto says. “People have a tendency to downplay the significance of the injury because they just don’t understand how such a seemingly mild impact could be serious.”
The best therapy depends on details of an accident – head position, speed, direction and type of vehicle – the severity of damage and a patient’s age and overall health. Whether or not a driver anticipates a collision and braces for it also can affect which neck structures sustain trauma.
Options include anti-inflammatory medications, muscle relaxants and heat or ice applications; physical therapy and tailored exercises and stretches; manual therapy; ultrasound or electrical stimulation; and dry needling, a technique that targets specific trigger points to release tension.
“Sometimes, it’s also about just making sure they’re not afraid to move their neck,” says Ken Morris, a physical therapist with Tidewater Physical Therapy in Newport News. “The first 24 to 48 hours often should be ice, heat, medication and rest, but then – if a doctor says it’s OK – they need to start to move. Even if it’s just to go up and down, and left and right, once each hour.”
Immobilizing neck collars generally “should only be used, if at all, for a brief time in the most acute phase,” Pinto adds, or in very severe cases.
Patients with more serious injuries also can benefit from epidural steroid injections or anti-inflammatory injections into specific joints of the spinal column, called facet joints. Another choice is radiofrequency ablation, or RFA, which burns nerves that feed damaged joints. RFA can block pain for eight to 10 months, allowing patients to participate more fully in physical therapy, Bradley says.
The goal should always be to go after the source of pain, not just mask it with indefinite, one-size-fits-all drugs, specialists say.
“Mild cases can resolve with the right type of medicine and exercises, but sometimes you really have to be a detective,” Bradley says. “The quicker we get beyond a ‘Band-Aid’ approach, the better.”