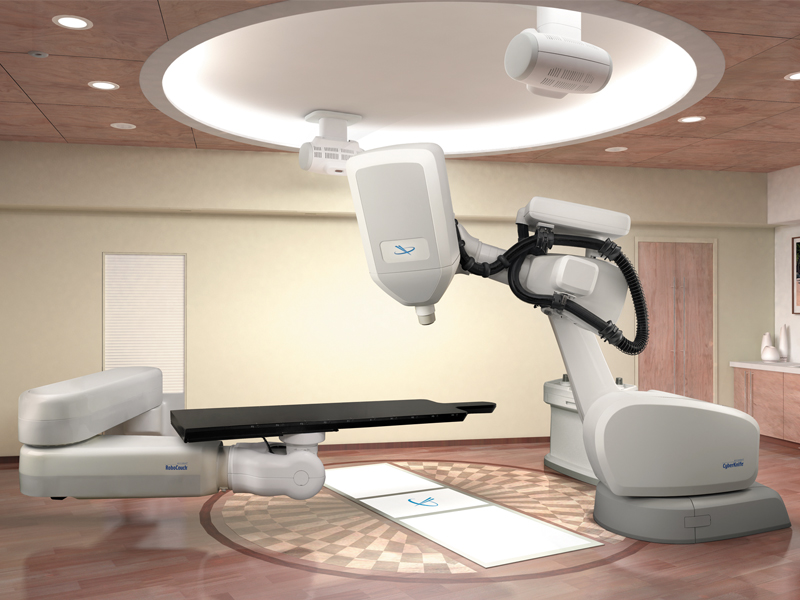
CyberKnife targets and zaps cancerous tumors
When Bob Davis first found out that he had lung cancer, he was understandably devastated.
Nearly 10 years prior, the North Carolina man had successfully gone through treatment for throat cancer. But lung cancer—that was some scary stuff. He didn’t know if he was up for having chemotherapy and radiation again.
Then he found out about the CyberKnife at the Sentara Advanced Radiosurgery Center at Norfolk General Hospital. The robotic radiosurgery system, one of the few in Virginia, offered a non-surgical procedure that had great results at getting rid of early lung tumors.
So Davis signed up. In February 2013, he went under the CyberKnife—a computer-controlled device capable of delivering radiation with pinpoint accuracy. And after three sessions, Davis was cancer-free. A year later, he remains that way.
“It’s unbelievable,” says Davis, 59. “This is where cancer treatment needs to go. It’s so exciting that it’s there.”
Sentara began operating its CyberKnife in January 2008, representing what Sentara physician Dr. Mark Sinesi calls “the evolution of radiation oncology. It has proved especially successful at treating early stage lung cancer, tumors in the spine, and in cases where cancer has spread to the brain, sparing more invasive surgery.
“It’s really been a new lease on life for brain-tumor patients,” says Sinesi, who is chairman of radiation oncology and biophysics at Eastern Virginia Medical School in Norfolk, Va.
A computer-controlled robotic arm originally designed to weld cars together, CyberKnife is driven by image-guided software—patterned after that used for cruise missiles—that allows doctors to zero in on the smallest of tumors. It can be used nearly anywhere on the body, on both cancerous and non-cancerous tumors.
Because the beams are so concentrated, damage to surrounding tissue is minimal. That means no burns. Some patients have even reported having less pain after the procedure. The motorized table that patients lie upon even rocks gently during treatment, mimicking breathing and eliminating the need to hold one’s breath for a radiation blast.
For lung cancers caught early enough, use of the CyberKnife gives a near 90 percent chance of surviving at least 10 years without any reoccurrences, Sinesi says.
“It’s remarkable,” says Sinesi who, has patients on the machine every day, all day.
Sentara’s CyberKnife is one of only three in the state, according to CyberKnife’s website. The other two are at hospitals in Roanoke and in Arlington. Beyond that, patients would have to travel to Washington, D.C., Baltimore, Md., or Chapel Hill, N.C.
Davis, who lives in Currituck County, traveled to Norfolk to meet with Sinesi while exploring options for treatment. Surgery would have likely meant removing a quarter of his lung, in addition to radiation and chemotherapy. But Sinesi thought Davis was a good candidate for CyberKnife.
So last February, Davis spent three 90-minute sessions reclined on a hospital bed while CyberKnife worked around him. The device blasted 187 beams at a 21/2-cm area in his upper left lung.
The machine, housed in a softly lit room in Norfolk General, plays spa music through the speakers unless a patient requests his own. Davis, who manages a radio station in the Outer Banks, made three playlists for each of his sessions, including songs such as John Mayer’s “War of My Life” and “I Will Survive” by Gloria Gaynor.
Although CyberKnife is typically not the first line of attack against cancers that require more comprehensive radiation, such as cancers of the breast, head and neck, Sinesi says there’s a growing need for it as time goes on. It delivers higher doses of radiation to stubborn spots.
Davis wanted to know what would happen if the cancer came back. Sinesi, he says, was reassuringly upbeat.
“He said, ‘We’ll just zap it again,’” Davis recalls. “We’ll kill this thing.”